In the rapidly evolving medical landscape of 2026, the treatment of chronic joint disease has moved beyond simple symptom management. For decades, the medical community viewed joint degradation as an inevitable decline—a slow, irreversible path toward immobility. However, breakthroughs in molecular biology have identified a specific biochemical “off-switch” that prevents joints from healing themselves.
Current research into 15 pgdh osteoarthritis mechanisms has revealed that our joints do not simply “wear out”; they lose their innate ability to repair due to enzymatic interference. By targeting this specific enzyme, scientists are unlocking the body’s hidden potential to rebuild cartilage from within, marking a new era where we restore function rather than just masking pain.
The Biological ``Off-Switch`` for Regeneration
The Role of the ``Gerozyme``
The enzyme known as 15 pgdh (15-hydroxyprostaglandin dehydrogenase) acts as the primary antagonist to this process. Its sole function is to break down and neutralize PGE2.
-
Age-Related Spikes: As we age, or following significant joint trauma, levels of 15 pgdh rise dramatically.
-
Regeneration Fatigue: This spike leads to a chronic PGE2 deficiency, effectively “muting” the body’s regenerative signals.
-
Permanent Damage: When these signals are silenced, the cartilage begins to thin, friction increases, and the clinical symptoms of arthritis become permanent.
Emerging Therapies: The Rise of the 15 PGDH Inhibitor
Why This Differs from Traditional Medicine
Unlike traditional anti-inflammatory medications, which often suppress a wide range of prostaglandins (including the beneficial ones), these specific inhibitors are surgical in their precision.
-
Cellular Rejuvenation: When the enzyme “brake” is removed, chondrocytes (cartilage cells) begin to behave like younger cells.
-
Matrix Synthesis: These rejuvenated cells start synthesizing type II collagen and proteoglycans, the essential building blocks of healthy cartilage.
-
Structural Improvement: For the patient, this means the possibility of moving beyond temporary relief toward a measurable structural improvement of the joint itself.
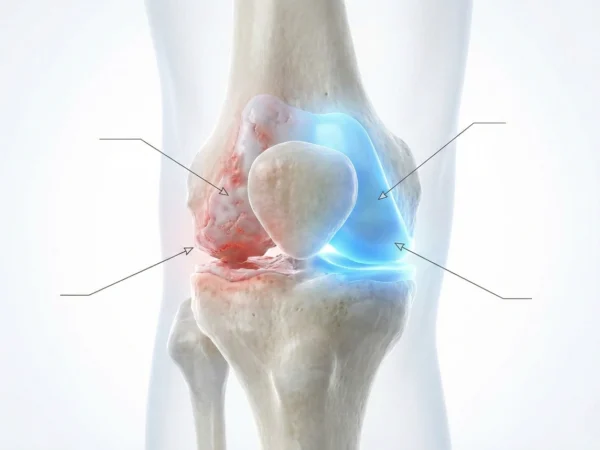
Understanding Joint Distress and Pathogenesis
Primary Causes of Knee Inflammation
Several factors can trigger the upregulation of 15 pgdh, leading to localized distress:
-
Mechanical Stress: Repeated high-impact activity that creates micro-traumas in the cartilage surface.
-
Metabolic Imbalance: Systemic changes that alter the biochemical environment of the joint fluid.
-
Post-Traumatic Changes: Previous injuries to the ACL or meniscus that disrupt the joint’s structural integrity.
-
Chondromalacia Patella: This condition, involving the softening of the cartilage on the underside of the kneecap, is often a precursor to advanced osteoarthritis.
The Treatment Spectrum: From Lubrication to Regeneration
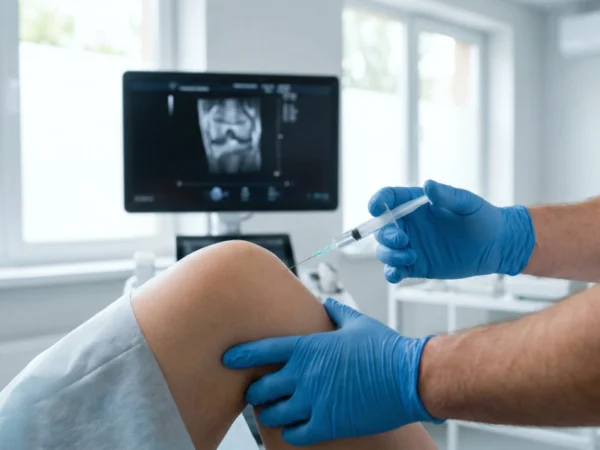
Before the advent of 15-PGDH research, the standard of care relied heavily on mechanical supplementation. The most common treatments, such as hyaluronic acid injections, remain vital tools in the orthopedic toolkit.
Hyaluronic Acid vs. Biological Inhibitors
Hyaluronic acid injections act as a “liquid cushion,” providing lubrication and reducing immediate friction between the femur and the tibia.
| Feature | Hyaluronic Acid Injections | 15-PGDH Inhibitors |
| Primary Goal | Lubrication and shock absorption | Cellular regeneration and repair |
| Duration | Temporary (months) | Potential for long-term structural change |
| Mechanism | Mechanical / Physical | Biochemical / Molecular |
| Best For | Immediate friction reduction | Stopping disease progression |
In 2026, the most effective protocols combine these methods. Using a lubricant to reduce mechanical wear while simultaneously using a regenerative agent to stimulate growth creates a synergistic effect that was previously unattainable.
Surgical Realities: When is Replacement Necessary?
Despite the massive leaps in regenerative medicine, there are instances where biological damage is too extensive for the body to repair, even with enzymatic help. When the cartilage has completely worn away, leaving no cellular foundation, a knee replacement becomes the most viable option.
The Evolution of Knee Surgery
A total knee joint surgery replacement is a highly refined procedure that involves removing damaged bone ends and replacing them with precision-engineered components.
-
Robotic Precision: Modern knee joint surgery replacement in 2026 utilizes robotic assistance for perfect alignment, reducing recovery times significantly.
-
Last Resort: While a knee surgery replacement is a radical step, it remains a critical “safety net” for patients who have reached end-stage joint failure.
The ultimate aim of 15-PGDH research is to make these surgeries the exception rather than the rule. By treating the biochemical environment early, we can preserve the natural biological joint for decades longer.
Living with Osteoarthritis in 2026
As we move forward, the focus is clearly on “biological youthfulness.” We have moved past the era where we accepted joint decay as a normal part of getting older. By targeting the 15 pgdh enzyme, we are addressing the root cause of why our bodies stop fixing themselves.
Proactive Management Strategies
For patients living with joint pain today, a multi-pronged approach is recommended:
-
Early Intervention: Addressing symptoms of chondromalacia patella before they transition into full-scale arthritis.
-
Inflammation Control: Identifying the specific causes of knee inflammation through advanced diagnostic imaging.
-
Biological Support: Utilizing inhibitors and lubricants to maintain the “molecular health” of the synovial fluid.
Conclusion: A New Chapter for Mobility
The identification of 15 pgdh osteoarthritis triggers has opened a door that was previously locked. It represents a transition from a world of “management and limitation” to one of “restoration and activity.”
Whether through the early use of a 15 pgdh inhibitor, the strategic application of lubricants, or the refined precision of a knee replacement, the goal remains the same: to keep the human body moving naturally and pain-free. The era of regenerative orthopedics is no longer a distant dream—it is the reality of modern medicine.